What is Osteomalacia?[]
Osteomalacia refers to a softening of your bones, often caused by a vitamin D or calcium deficiency. Soft bones are more likely to bow and fracture than are harder, healthy bones. It is the weakening of the bones. Problems with bone formation or with the bone building process cause osteomalacia. Osteomalacia isn’t the same as osteoporosis. Osteoporosis is a weakening of living bone that has already been formed and is being remodeled.
How does Osteomalacia Affect the Skeletal System?[]
Osteomalacia is caused by a dysfunction in the bone-building process. Because vitamin D is needed to build strong bones, any disorder that affects vitamin D, calcium, or phosphorus levels in your body will affect your bones by softening, and causing cracks. By this it affects the skeletal system since this disease is weakening and softening your bones, with the lack of vitamin D, the skeletal system is incapable of distributing the nutrients that your bones need. Soft bones are more likely to bow and fracture than are harder, healthy bones.
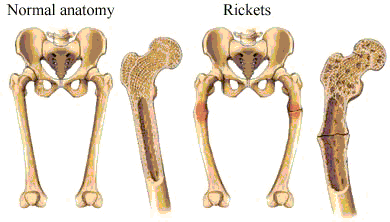
Signs and Symptoms[]
- Bones that fracture very easily are the most common symptom.
- Another symptom is muscle weakness. This happens because of problems at the location where the muscle attaches to bone. ...
- Bone pain, especially in your hips, is also a very common symptom.
- Muscle pain is also very common if the muscle is directly connected to the bone that is softening.
The pain of Osteomalacia sets in very quickly, but it all depends on the severity of your case. If you have Osteomalacia, you will have one of these symptoms at the least and as your condition worsens, you will notice more symptoms.
Diagnosis[]
Your body uses calcium, vitamin D, and phosphate to build strong bones. Osteomalacia may occur if you don't get enough of these minerals and calcium in your diet or if your body doesn't absorb them properly. Osteomalacia is caused by lack of calcium, phosphorus, and most commonly caused by a lack of vitamin D. Vitamin D is an important nutrient that helps you absorb calcium in your stomach. If this calcium is not absorbed, then there becomes a deficiency of vitamin D which deprives the bones of nutrients, causing them to weaken, and soften. Some ways to test if someone has osteomalacia is to take blood and urine samples for testing. In cases of osteomalacia caused by vitamin D deficiency or by phosphorus loss, abnormal levels of vitamin D and the minerals calcium and phosphorus are often detected. There is also X-ray. Slight cracks in your bones that are visible on X-rays — called Looser transformation zones — are a characteristic feature of people with osteomalacia. Bone biopsy. During a bone biopsy, your doctor inserts a slender needle through your skin and into your bone to withdraw a small sample of bone marrow for viewing under a microscope. This procedure is done after using a local anesthetic and takes only about a half-hour. Although a bone biopsy is very accurate in detecting osteomalacia, it's not often needed to make the diagnosis.These tests will be testing you are low on calcium, vitamin D, and phosphorus.
Treatment[]
If osteomalacia is detected early, treatment can be as simple as taking oral supplements of vitamin D, calcium, or phosphorus. If you have absorption problems due to intestinal injury or surgery, or if you have a diet low in key nutrients, this may be the first line of treatment.
These supplements are very beneficial and help heal your bones from the damage of osteomalacia. Although, if you want to fully recover, you have to take supplements everyday or else they will be ineffective.
Osteomalacia
This disease occurs when the bones soften, it is typically caused by vitamin D or calcium deficiency. Sometimes it can be caused by certain surgeries, celiac diseases, kidney or liver disorders, and drugs. Osteomalacia causes the bones to be vulnerable, to bow and fracture. This disease results from a defect in the bone-building process. Symptoms are often muscle weakness, and aches and pains in the bones. This can be treated by replenishing low levels of vitamin D and calcium. Patients can be diagnosed using blood and urine tests, x-rays, and bone biopsies. Treatment of this disease requires in-taking vitamin D, calcium, or phosphorus supplements.